Intubation is an essential medical procedure performed to save a person’s life when they can’t breathe naturally. It is done by inserting an endotracheal tube (ETT) through a person’s mouth or nose, voice box, and trachea using a laryngoscope. The tube keeps the airway open. Intubation is an everyday yet critical medical procedure during emergencies such as cardiac arrest, lack of consciousness before specific surgeries, and neck and head injuries.
In this article, we will learn what is an endotracheal tube, its anatomy, types, application, and crucial significance during the intubation process.
What is an Endotracheal Tube?
1. Definition and Core Function
You may be wondering what is an endotracheal tube. Well, it means “Through the trachea.” An endotracheal tube (ETT) is a flexible tube usually made of polyvinyl chloride (PVC). It is inserted in the trachea through the mouth or nose to keep it open and establish an airway for oxygen and inhaled gasses while protecting the lungs from contamination, e.g., gastric contents and blood. The tube then connects to an external machine that provides oxygen support.
The core function of an endotracheal tube is to provide mechanical ventilation and breathing support to patients before surgery, lung and chest trauma, and air obstruction problems.
2. Components of an Endotracheal Tube
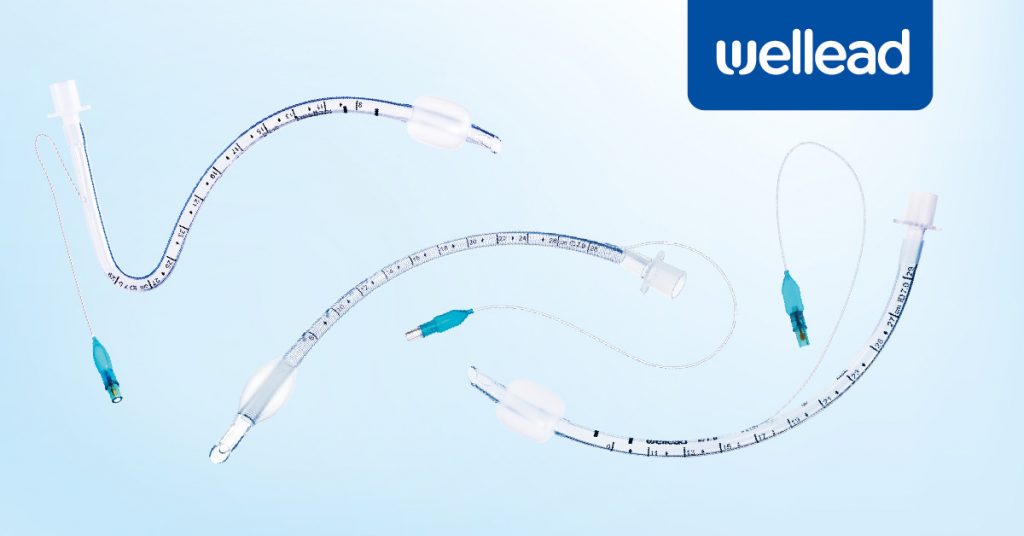
Having established a basic understanding of what is an endotracheal tube, let’s move on to its core components and functions. The diameter of the tube is determined by its internal diameter, typically measured in millimeters. The bevel, a slanted portion at the tube’s tip, aids in visualizing vocal cords during intubation. Murphy’s eye, an opening above the bevel, ensures ventilation in case of bevel obstruction. The cuff, a balloon attached to the tube, reduces secretions and facilitates oxygen supply, while the pilot balloon and one-way valve control cuff inflation. Finally, an adapter (15mm) at the tube’s other end allows connection to a ventilator or Ambu bag for oxygen supply.
3. What is An Endotracheal Tube: Major Types
Oral Endotracheal Tube
A standard endotracheal tube with all components, as explained above. Oral endotracheal tubes are used for general purposes and head and neck surgeries.
Nasal Tracheal Tube
Nasal tracheal tubes are for people who need prolonged intubation. They are placed into the nostrils and gently moved towards the trachea through the nasopharynx.
Reinforced Endotracheal Tube
Armored or reinforced Tracheal tubes come with a reinforced metal coil inside. They are less likely to get compressed or blocked. Making them an ideal choice during complex surgeries.
Applications of Endotracheal Tubes
Now that we have developed a comprehensive understanding of what is an endotracheal tube and its types, let’s explore its applications in different medical conditions and procedures:
• General Anesthesia: Endotracheal tube intubation is the most commonly used airway during general anesthesia.
• Emergency Intubation: They are used during emergency intubations when a person is under a non-threatening respiratory compromise that can turn into a life-threatening situation later.
• Mechanical Ventilation: Providing life support to patients who can’t breathe independently due to a critical illness.
• Respiratory Distress Syndrome: When fluid builds up in the tiny air sacs (alveoli) of the lungs, and it is impossible to breathe naturally without intubation support.
• Postoperative Recovery: During the postoperative recovery phase, until the functions are restored and adverse symptoms of a patient are fully resolved, additional breathing support is given through endotracheal intubation.
• Neonatal And Pediatric Care: premature newborns or babies born with low birth weight. Infants with poor perfusion or in cardiac arrests or airway obstructions are given respiratory support through intubation.
• Bronchoscopy And Diagnostic Procedure: Endotracheal intubation is also done during specific diagnostic tests, such as bronchoscopy, to detect tumors, abnormal airways, or lung cancer.
The Intubation Process
Knowing what is an endotracheal tube might have seemed a vague concept. However, here’s a comprehensive endotracheal intubation process:
1. Pre-Intubation: Sedation and Paralysis
• A healthcare professional inserts an IV into the patient’s arm and gives medications to keep the patient sedated during the procedure.
• Oxygen is given with the help of an oxygen mask to increase blood saturation levels.
2. Intubation
• During the intubation process, the healthcare practitioner stands towards the head of the table, looking towards the feet of the patient. A pillow or padding is sometimes placed under the patient’s head to make the procedure easier.
• A laryngoscope is inserted into the patient’s mouth; the tool has a small light that helps locate the practitioner’s tracheal tube.
• Once the proper placement is determined through lung and abdominal sounds, the practitioner raises the epiglottis with the help of a laryngoscope, leading the tube to the larynx and then towards the lower trachea while holding the laryngoscope.
• The balloon cuff is inflated to make sure the tube stays in the right place and the air given reaches the lungs.
• A tape is placed on the sides of the patient’s mouth to avoid slipping the tube.
3. Mitigating Complications and Monitoring Patient’s Responses
The process of intubation is generally safe. However, there could be some associated complications and risks that healthcare practitioners should carefully monitor.
• The laryngoscope should be handled carefully in the mouth and trachea to avoid tracheal bleeding, dental and oral injuries, and mouth sores.
• Prolonged intubation can lead to cartilage thinning and narrowing air passage.
• The tube should not enter into the esophagus of the patient under any circumstances; it can result in brain damage and sometimes immediate death.
4. Removal of Endotracheal Tube
A healthcare practitioner carefully assesses the patient to check if it is safe to remove the intubation and if the patient can breathe independently.
• The tape holding the tube in place is removed.
• A suction device is used to clean any debris or residue.
• The balloon is deflated.
• The patient takes a deep breath or exhales while the health practitioner removes the tube.
• It may feel odd to have a sore throat or an uncomfortable feeling for a few days, which is normal.
Endotracheal Tubes: Well Lead Medical’s Approach
Well Lead Medical has a comprehensive approach to premium quality endotracheal tubes, making us a trusted endotracheal tube manufacturer. We have a range of intubation accessories covering all aspects of patients’ needs and their diverse medical treatments.
Well Lead Medical makes all significant types of endotracheal tubes, such as oral, nasal, and reinforced endotracheal tubes. Some of their prominent features are:
• Radiopaque Line: These tubes come with a high-quality radiopaque line that enables the correction position of the endotracheal tube in the trachea with the help of an x-ray.
• 15 mm Connector: A 15 mm connector connects with all modern ventilating equipment without hassle.
• Versatile Cuffs: Available with high volume, low-pressure cuffs, low profile cuffs, and uncuffed according to the individual needs of every patient.
• Wire Coil: The reinforced endotracheal tube has a wire coiling that increases flexibility and provides kink resistance.
The extensive size range of these endotracheal tubes caters to the needs of all ages and genders, making them a popular choice.
Conclusion
Intubation is a very common medical procedure that saves a person’s life when they can not breathe by themselves. This article aimed to provide a detailed understanding of what is an endotracheal tube, its components, functions, and significance in medical procedures. To perform all these medical procedures, you need robust and reliable equipment, and that’s where Well Lead Medical shines.

